|
We present a woman with unilateral sudden sensorineural hearing loss, tinnitus, disequilibrium, and vertigo who was mistakenly diagnosed with a vestibular schwannoma and referred to our institution for radiosurgery. Theories to explain this phenomenon include elongation of arteries with age, arteriosclerosis, development of arachnoid adhesions between the artery and nerve, and hypoxic damage to the cochlea and vestibular system due to arterial compression. There is also uncertainty as to why these symptoms manifest in some patients with AICA loops in the IAC but not others. While some studies demonstrate a correlation between symptoms related to microvascular compression of the VCN complex and VCN dysfunction, others do not recognize this correlation and classify AICA loops within the IAC as normal variants. Hemifacial spasm is an accepted clinical sequela of vascular compression of the facial nerve. 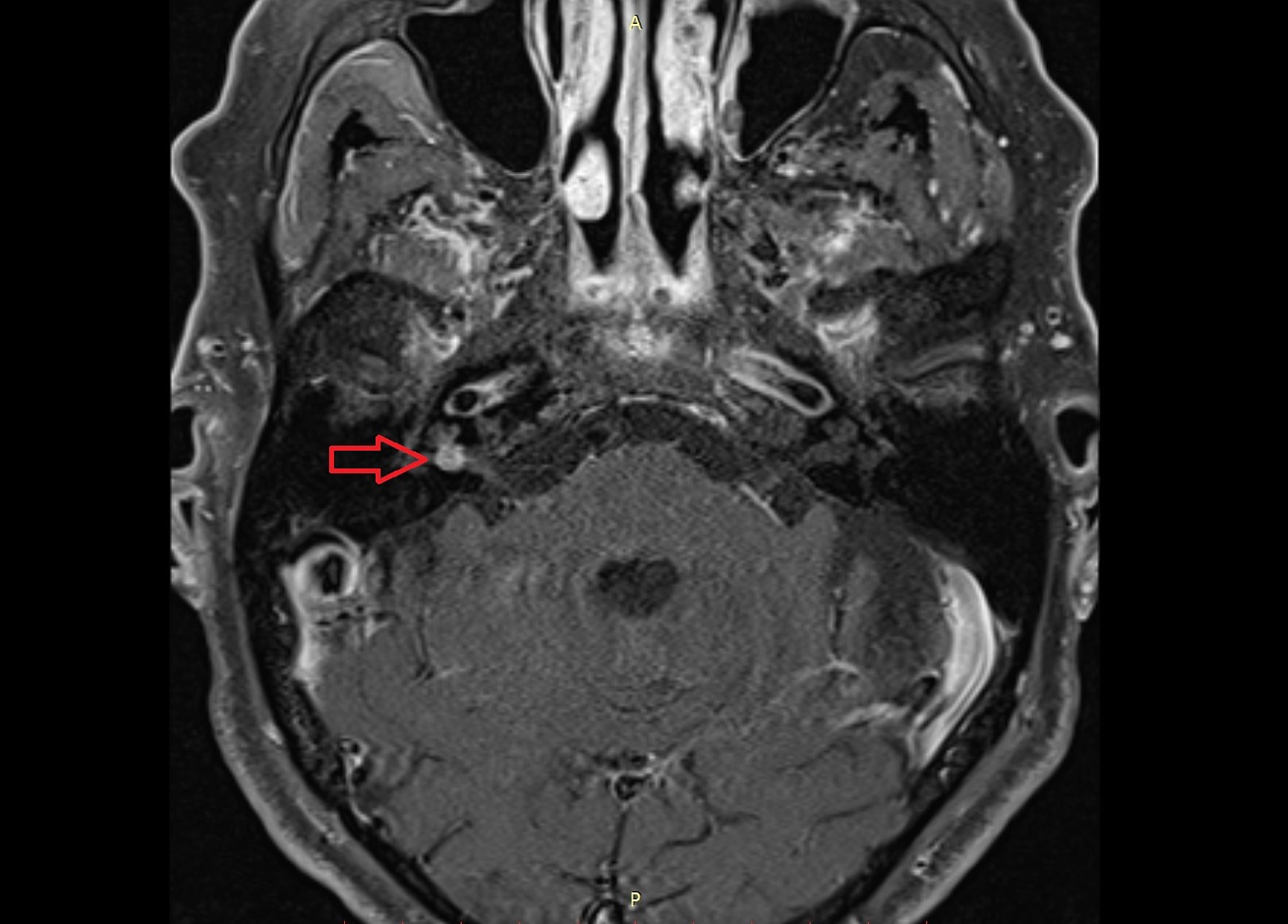
In 1975, Janetta proposed that compression of the VCN by the AICA within the IAC could be responsible for symptoms of hearing loss, tinnitus, vertigo, and hemifacial spasm however, this has been a point of much controversy. These more unusual lesions can lead to confusion in diagnosis due to the similar symptomatology and MRI findings of vascular compression of the VCN. However, there are other causes for cranial nerve dysfunction in this area – both neoplastic and non-neoplastic such as compression from vascular malformations and arterial loops. Patients with VS commonly present with progressive unilateral sensorineural hearing loss and tinnitus, but can also present with SSNHL, symptoms of vestibular dysfunction, facial numbness/pain, and facial paresis. The most common pathology of the VCN in the CPA and IAC is a vestibular schwannoma (VS), a neoplasm of Schwann cells that is responsible for 5-10% of all intracranial tumors. The prevalence of AICA loops within the IAC has been reported to be between 13-40% in post-mortem dissections and 14-34% by magnetic resonance imaging (MRI). There is high variability in the course of the AICA within the CPA. A terminal artery, the labyrinthine artery is the sole blood supply of the labyrinth and an area of the brainstem and cerebellum. It gives rise to the labyrinthine (internal auditory) artery, which supplies the cochlea and vestibular system. The anterior inferior cerebellar artery (AICA) arises from the basilar artery and courses variably posterolaterally in the CPA or along the underside of the cerebellum supplying the anterior cerebellum including the flocculus, middle cerebellar peduncle, and inferolateral pons. Anterolateral to the CPA, the internal auditory canal (IAC), a bony channel situated along the posterior face of the petrous bone, transmits the facial nerve from the CPA to the temporal bone and ultimately the face, and the vestibulocochlear nerve (VCN) from the cochlea and vestibular apparatus to the brainstem. The CPA contains cranial nerves V-VIII, the superior cerebellar artery (SCA), anterior inferior cerebellar artery (AICA), and draining veins. The cerebellopontine angle (CPA) is a cerebrospinal fluid-filled, triangular space located at the junction of the lateral pons and anterior cerebellum. She was not offered radiosurgery, and she elected conservative management. There was no evidence of a schwannoma on the repeat MRI. Repeat MRI demonstrated a loop of the anterior inferior cerebellar artery (AICA) compressing the vestibulocochlear nerve within the right IAC. She was originally diagnosed with a vestibular schwannoma on magnetic resonance imaging (MRI) and was referred to our institution for Gamma Knife radiosurgery. The current report represents an attempt to understand this clinical entity as discussed in the current literature.Ĭase summary: A 77-year-old female with a long history of progressive right-sided hearing loss and episodic vertigo developed unilateral right SSNHL, tinnitus, vertigo, and disequilibrium. Underlying pathophysiologic factors surrounding microvascular compression of the vestibulocochlear nerve are poorly understood and make treatment recommendations, especially the option of microvascular decompression, difficult if not controversial. We present a patient with unilateral sudden sensorineural hearing loss (SSNHL) who was found to have a vascular loop in the ipsilateral internal auditory canal (IAC), and we review the literature regarding this association.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
